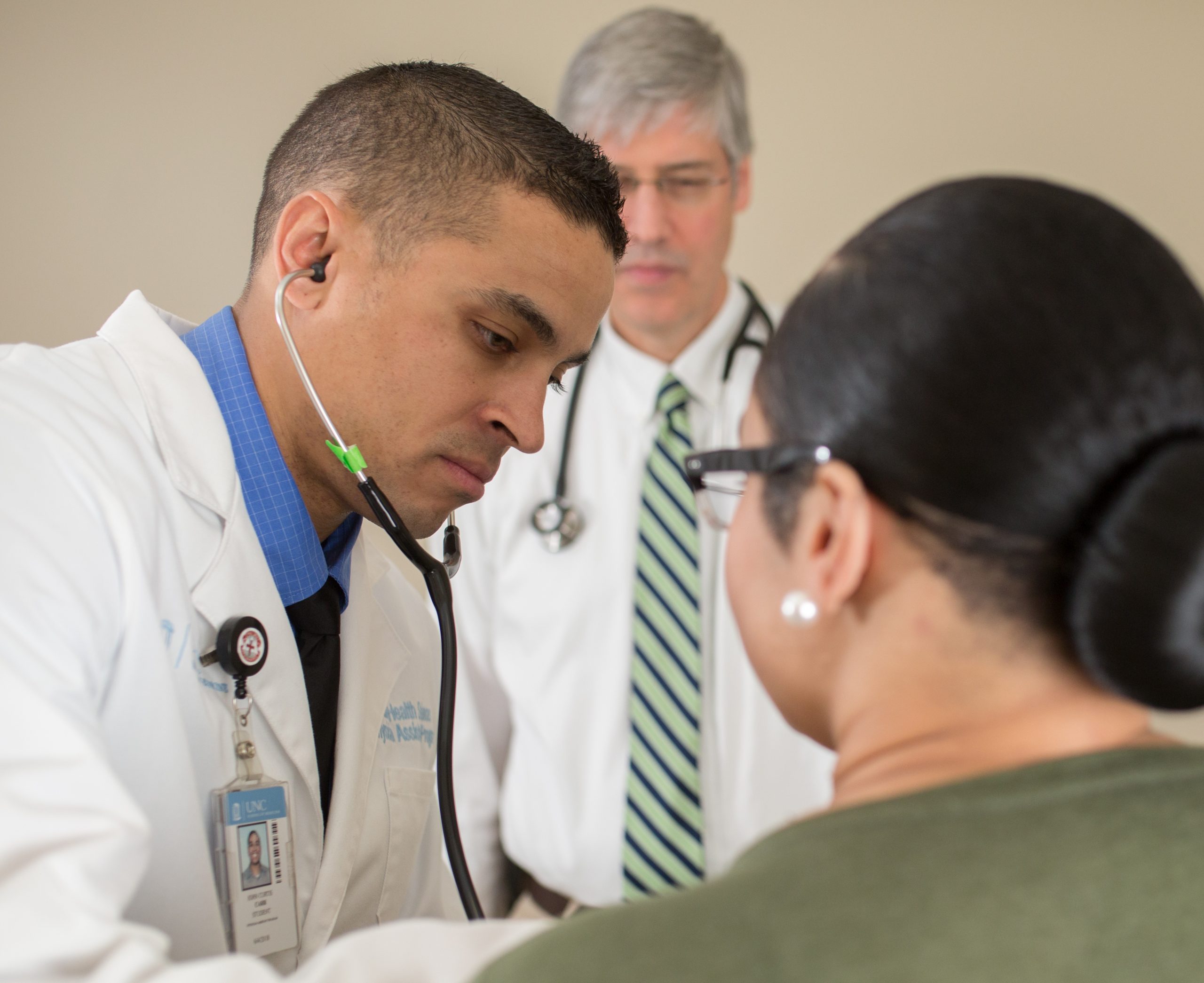
As a student in the UNC School of Medicine’s Physician Assistant Program, two-time Bronze Star Award recipient Curtis Carr is building on the medical skills he acquired as a Green Beret medic serving in Afghanistan. He looks forward to applying these skills in the civilian world next year.

As a student in the UNC School of Medicine’s Physician Assistant Program, two-time Bronze Star Award recipient Curtis Carr is building on the medical skills he acquired as a Green Beret medic serving in Afghanistan. He looks forward to applying these skills in the civilian world next year.

by Zach Read – zachary.read@unchealth.unc.edu
In September 2014, Curtis Carr was at home, in Whispering Pines, North Carolina, on a break between Special Forces combat deployments in Afghanistan. His wife, Suzi, a nurse practitioner at Moore Family Medicine, in nearby Carthage, was pregnant, about to give birth to their second son, Augustus.
As a Green Beret medic – or 18-Delta – it was unusual for Curtis to be home. Military commitments forced him to be away for so much of the three years he and Suzi had been married and the two years since they’d had their first son, then-two-year-old Grayson.
“As a Special Forces guy, and with all the extra training I’d done as a medic and a dive-company member, I was home only a quarter of the year,” explains Curtis, a second-year student in the UNC Physician Assistant Program and a member of the program’s inaugural class. “It was hard on all of us.”
And dangerous for Curtis and his Special Forces unit. Deployments in Afghanistan included continuous conflict with Taliban forces in the mountain regions near Kabul. In total, he was involved in more than 120 firefights. The experiences – and his actions during them and throughout his deployments – earned him two Bronze Stars. Training and requalification for his military role, meanwhile, required him to take Special Forces Combat Diver and Dive Medical Technician courses in Key West, Florida, and other locations. Every time he trained or requalified, he was one mistake away from an arterial gas embolism or decompression sickness – a.k.a. the bends – and he could never rule out the possibility of an encounter with an ocean predator or the potential for unpredictable weather conditions while deep in seawater.
Yet, despite years of strenuous military commitments, he was present for the births of both of his sons.
“Being a father is the most important part of my life,” he says. “My father was there for me and my brother, so I understand how important it is to be around. I wouldn’t be where I am today without that support.”
That September, Augustus was delivered at FirstHealth Moore Regional Hospital, in Pinehurst. Hours after his birth, he was having trouble breathing. At 3 a.m., the situation seemed stable, so Curtis drove home to pick up a change of clothes. By the time he returned to the hospital, however, something was wrong.
“When I looked at Suzi I could tell there was an issue,” he remembers. “She was distraught.”
Augustus had been rushed to the NICU because he wasn’t breathing well on his own. He would spend the next week under close watch by NICU caregivers – the experience changed Curtis’s life.
“The providers allowed us to be there with him while they cared for him,” he recalls. “I’ve performed a lot of difficult trauma care in my life and prepared for a lot of challenging situations. Nothing prepared me for this. It scared the life out of me. Seeing my son like that was the moment I decided to change my career – I needed to do something that would keep me with my family.”
Becoming an 18-Delta
After graduating from high school in Colorado, Curtis joined the Navy. But a vision issue in one eye led to his discharge. Years later, in 2007, he was waiting tables in Brooklyn, New York. He’d just graduated from college and was living with his father, an associate warden at Metropolitan Detention Center Brooklyn.
“I waited on some service members, and we began talking about the military,” Curtis says. “They thought I’d be a great fit because of my athleticism and willingness to become a Combat Medic, and the military needed bodies at that time.”
Physically, Curtis would excel in military training. He’d always been an athlete, and he’d come from an athletic family. His father played small forward for the University of Tennessee-Martin men’s basketball team, and his uncle Chris played seven years in the NBA, a stint that included an all-star weekend dunk contest finals matchup against Kobe Bryant in 1997. Curtis also played basketball – at Otero Junior College, in Colorado, and at Northern State University, in South Dakota, under Hall-of-Fame head coach Don Meyer.
“I was ready from a physical standpoint,” he says. “But I think the military was as interested in how I performed on my aptitude tests, including the ability to learn a foreign language.”
Curtis joined the U.S. Army, and his first report was for basic training at Fort Leonard Wood, in Missouri. Upon arriving, his goal was to be a 68 Whiskey, or combat medic, which would take him to Fort Sam Houston, in Texas, for further training. As an undergraduate student at Northern State, he recalls Coach Meyer asking him what he wanted to major in – his answer was something he could now apply in the military.
“So many of my teammates wanted to go into coaching,” he says. “I love basketball, but I didn’t love it enough to make it my life. So I majored in chemistry, and I knew I wanted to somehow be around medicine. 68 Whiskey seemed perfect for me.”
In basic training, Curtis did so well that his drill sergeant spoke with him privately about becoming a Green Beret.
“It was a surprise to have that conversation so quickly, during the second week of basic training,” he says. “I didn’t know what a Green Beret was, but after learning more about it, I was excited about the possibility becoming one. Without telling me, he started my Special Forces packet.”
Because of his late interest in Special Forces, he’d have to take a nontraditional route to get there. After basic training, he reported for Advanced Individual Training at Fort Sam Houston, where he learned to be a 68 Whiskey. While there he was one of two soldiers – out of 480 – who qualified for Airborne training school in Fort Benning, Georgia, a required step for the Special Forces Assessment and Selection Course. Curtis completed Airborne training and was transferred to Fort Bragg in September 2008. Two months later, he began Special Forces assessment and selection, followed by nine weeks of Small Unit Tactics School and several more weeks of survival school.
“Special Forces training was the roughest period of my life,” he says. “I lost 25 pounds – not because they didn’t feed us, but because they kept us up 19 to 22 hours a day while also doing strenuous physical work. They want to see how you function when you’re tired, because you don’t always get to decide when you have to work during operations, and you can’t always predict what circumstances you’ll face in the field.”
An 18-Delta is the medic on the Green Beret Unit. The Alpha is the officer, the Bravo is the weapons expert, the Charlie is the engineer, and the Echo is the communications expert. Deltas require additional, more time-consuming training than the other team members. After completing his initial Special Forces training – and being selected – Curtis learned how to provide acute trauma care and other medical care in austere environments. Part of that training, outside of the Joint Special Operations Training Center at Fort Bragg, included honing his skills in clinical rotations at VCU Medical Center’s Emergency Department, in Richmond, Virginia.
At VCU, he split time between the emergency room and the ambulance, servicing trauma patients by inserting chest tubes and performing other airway-related procedures. The medical students and residents he learned alongside took notice of the quality and speed of his work.

“They watched me and would ask, ‘Who are you again?’” he laughs. “I was through two chest tubes before one medical student could even make the cut. All I’d done the previous eight months was this type of medical work. I was aggressive, strong, fast, and smart. For me, doing those rotations reinforced that I wanted to be in medicine throughout my life.”
In the Field
Curtis had the option of three types of Special Forces companies in which to serve as an 18-Delta. He chose combat diver. To be a combat diver, he had to train for SCUBA – first in a pool at Fort Bragg, then in the open ocean off Key West.
“We’d do drown-proofing exercises in the water to the point of exhaustion, incorporating stress events, getting your heart up to 130 beats per minute,” he explains. “Eventually, we were diving 120 feet below the surface, performing both open- and closed-circuit diving.”
He admits he wasn’t the best in the water – but he was good at handling the fear: “I might have been one of the worst in the water, but I was calm. I could keep the panic at a manageable level. Some people aren’t able to do that – it’s just impossible for them. But with 120 feet of seawater above you, if you panic, you may die.”
The physical training of a combat diver prepared him for the physical nature of his role in Afghanistan.
“In my first deployment, we climbed mountains for nine months,” he jokes.
His unit served as force multipliers – producing outsized outcomes for a unit of only 12 individuals. During his deployments, they trained the Afghan National Police in the administration of basic first aid, improved the police’s limited medical capability, and enhanced their police skills so that they could stand up to the Taliban. After training the Afghans, Curtis’s unit joined them in the field, where they immediately faced resistant Taliban forces.
“We’d show back up with newly trained police forces, to the roughest part of the country, and our trainees would exert their authority, while the Taliban would say, ‘We’re in charge,’” he says. “The conflict was constant.”
They endured road bombs, gunfights, and grenades hurled at them. Some fights lasted for several days. Six members of his unit died during his first deployment in 2012.
“It was difficult for everyone,” he says. “Those are your guys. One minute they’re standing right next to you and the next minute they’re being rushed by helicopter to wherever they could get the next level of care. As a medic, you’ve done everything you can do to stabilize them and get them medically evacuated, and you pray that they live. But unfortunately, too often you later find out they didn’t.”
A Voracious Learner
Soon after Augustus’s stay in the NICU, Suzi, whom he met while she was a PACU nurse at VCU, told Curtis about the new PA program being launched through the UNC School of Medicine’s Department of Allied Health Sciences. The more he learned about its mission to incorporate veterans with medical experience – particularly 18-Deltas – the more he wanted to apply.

But to qualify he had to complete prerequisites, including biochemistry, microbiology, and medical terminology. Four nights a week, for several hours each night, he took the courses through Campbell University’s Fort Bragg campus. At the same time, he was a husband, father to two young boys, and a dive-medic technician, preparing future soldiers like him to go to Key West for more training.
“It was intense,” he says, “but I’d pushed myself before, and UNC seemed like it would be a place where my background would be valued.”
The UNC program launched in January 2016, and Curtis was part of its inaugural class. Of the class of 20 students, he and eight others have military experience. Together, the class has the largest number of clinical hours of any PA program in the United States. Despite their previous experience providing medical care, the students have had to work extremely hard since arriving on campus.
“They tell you that the first year of PA school is like cramming four years of medical school into a year, and I can say that felt true to me,” says Curtis, who, along with his classmates, is doing clinical rotations during his second year of PA school. “There’s a tremendous amount of information you need to know.”
Not surprisingly, he has brought the same approach to his studies that he did to Special Forces.

“Throughout the program, Curtis has been extremely assertive and voracious in his appetite for learning,” says Paul Chelminski, PA program director, professor of medicine, and primary care physician at UNC. “He takes questioning to the next level and is self-directed and independent as a learner. That is probably a byproduct of what made him a successful Green Beret medic. Green Berets are selected for these qualities of independence, rapid problem solving, initiative, and an ability to execute practical tasks, and Curtis has demonstrated these skills at UNC.”
Chelminski was particularly gratified at the beginning of the 2016 fall semester when he walked into the surgical skills class and saw Curtis and fellow veteran Richard Cowan assisting classmates in their exercise.
“What we hoped would happen in this new PA program was happening,” Chelminski continues. “Our veterans with medical experience have a range of skills, especially practical skills, and they were sharing these skills with other students. In this case, they were practicing suturing – sewing up simulated wounds on manikin extremities. Our veterans were assuming the role of teacher, and this kind of expertise – the kind exhibited by Green Berets in this academic environment – is an element unique to this PA program.”
PA school has not been without challenges, as transitioning from military to civilian life – and specifically to an academic setting like the UNC School of Medicine – requires assistance from others. The veteran students have been able to relate to one another about their experiences, helping each other put into perspective studying and exams by remembering the life-and-death situations they’ve faced. In addition to fellow students serving as resources, it helps to have individuals like Todd Williams, a former Green Beret medic who spent 28 years in the military, as a program faculty member and advisor.
“Todd has been such a huge help to the veterans during this transition for us, from military life to civilian life,” says Curtis. “In this academic world, there’s a very noticeable change in how you relate to people compared to what occurs in the military community. Todd has now been in both, and he advises us, helping us bridge the two. And at the most basic level, Todd is someone I can look up to.”
Williams refuses to take credit for the success of Curtis and his classmates with military experience.
“He’s taken this opportunity seriously and is an easy person to advise because of that,” says Williams, who served as a PA at Womack Army Medical Center when he wasn’t deployed in the latter part of his military career. “The only thing I’ve been able to bring to bear as an advisor are my own experiences on the transition from the military community to an academic environment. In the Special Forces, you’re a member of a team, which correlates well to what our students are learning about interacting in today’s interprofessional approach to medicine. At the same time, however, it’s important for our 18-Deltas, who are often the sole provider on the battlefield, to understand that they do not have to rely on their skills exclusively in the civilian clinical setting. Instead, they can step back and let someone else be the subject-matter expert.”
Curtis understands that medicine is more than the trauma patient he became so expert at caring for in the field. Relating to the patient – and understanding his or her complex needs – is his next challenge as a provider. He expects ongoing clinical rotations at UNC Hospitals, Hillsborough Hospital, and other locations to help him become a more well-rounded caregiver.
“I really enjoy seeing the patient – interacting with the person,” he says. “They are often at a low point when they come to see you. Something is wrong and they hope you can help them. For me, it’s both inspiring and rewarding hearing from them about their medical issues and being relied on to provide them the service they expect.”
The result of a public-private partnership that includes support from Blue Cross Blue Shield of North Carolina, the Kenan Trust, and several charitable foundations, the PA Program provides educational and career-development opportunities to nontraditional students, including military veterans with medical experience, who are committed to the program’s mission to reduce health-care shortages in underserved communities in North Carolina. Read more UNC PA Program news and stories: