CHAPEL HILL, NC – Heart disease continues to be the leading cause of death worldwide, partly due to limited therapeutic options and the heart’s inability to regenerate healthy cells called cardiomyocytes after heart attacks. Scientists at the UNC School of Medicine and elsewhere are exploring ways to reprogram scar tissue cells into healthy heart muscle cells, and now UNC researchers have published the first scientific paper to compare in great detail the two leading reprogramming techniques.
Led by Yang Zhou, PhD, a postdoctoral fellow in the laboratory of Li Qian, PhD, assistant professor of pathology and laboratory medicine at UNC, research published in Cell Reports suggests that one method leads to the creation of cardiomyocytes with genetic signatures that closely mimic those found in healthy adult heart muscle cells. The other reprogramming approach leads to the creation of cardiomyocytes with more embryonic cell signatures.
“The differences in the cardiomyocytes generated using these two methods are striking,” said Qian, who is also a member of the UNC McAllister Heart Institute. “Researchers can choose one or the other method based on the specific type of cardiac disease they are interested in studying, while clinicians could carefully select which method is best, considering the pros and cons of each approach.”
Cardiomyocytes, the cells responsible for the beating of the heart, are essential to repairing the heart after injury. But after injury, such as a heart attack, many of these cells are irreversibly lost; they’ve been turned into scar tissue cells. The replacement of these lost cells with patient-specific cardiomyocytes has gained attention as a potential therapy because existing healthy heart tissue better accepts these cells and because of increased recovery rates. Patient-specific cardiomyocytes also offer unique advantages for drug screens to help doctors identify each patient’s tailored drug type and dosage.
There are presently two widely practiced approaches to generate patient-specific cardiomyocytes.
In the first approach, an adult connective cell called a fibroblast is reprogrammed back into a naïve embryonic stem cell-like state. Once in this naïve state, the cell has the potential to develop into any cell type in the body, but researchers direct it to develop into a cardiomyocyte. These newly created cardiomyocytes are called induced pluripotent stem cell cardiomyocytes (iPSC-CM).
In the second approach called direct cardiac reprogramming, a fibroblast is directly converted into a cardiomyocyte, without having to first be reprogrammed into a naïve embryonic stem cell. These new cardiomyocytes are called induced cardiomyocytes (iCM).
Qian lab’s compared cardiomyocytes generated using these two approaches to the original starting cell type (cardiac fibroblasts) and to true cardiomyocytes. The researchers found that both methods resulted in cells with classic cardiomyocyte molecular features. However, by comparing the unique set of genes activated or not activated in each group of cells, the researchers found that iPSC-CMs more closely resembled embryonic cardiomyocytes, while iCMs more closely resembled adult cardiomyocytes.

“This is crucial knowledge,” Qian said. “When developing research projects or creating new therapies, we need to know these sorts of genetic features to best help patients.”
Researchers also found that iPSC-CMs feature more active genes and a higher number of genes poised to be either activated or repressed (known as “epigenetically hyperdynamic”), a trait more commonly found in potent cells.
Metabolically, iPSC-CMs had a higher expression of glycolytic genes while iCMs had a higher expression of genes involved in fatty acid oxidation, the primary means of energy production in adult hearts.
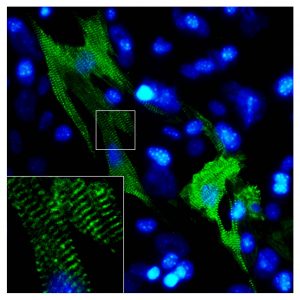
In iPSC-CMs, heart muscle cells called sarcomeres, which give the heart a striated look, were less organized than in iCMs. The contractibility of cardiomyocytes as measured by the intake and removal of calcium was also greater in iCMs, again suggesting that iCM cells are more mature than iPSC-CM cells.
Next, the researchers investigated if allowing iPSC-CMs to grow longer would increase their maturation. iPSC-CMs were collected at various time points and analyzed. Longer culture times increased the number of mature cardiomyocyte genes but did not decrease the number of embryonic cardiomyocyte genes. The sarcomere structure of iPSC-CM cells also improved with increased culture time but did not match the organization of iCM cells. This indicated that iPSC-CMs and iCMs take different routes to maturation.
”Although each method has pros and cons,” Qian said, “for congenital heart disease, iPSC-CMs might be ideal for the study of mechanism and for performing drug screens.”Surprisingly, one such reprogramming route may be dependent on cell-cycle status.
Adult cardiomyocytes do not enter the cell cycle, meaning they cannot replicate and produce more cells. This partly explains their inability to replenish the heart after injury. Fewer cell cycle genes were active in iCMs. Additionally, the researchers found that reduced expression of a common cell cycle gene in iPSC-CMs resulted in sarcomere organization more similar to adult hearts.
This study highlights the importance of considering various reprogramming techniques used when generating patient-specific cardiomyocytes. The chosen technique may affect the molecular characteristic of the cardiomyocytes generated. The best approach is likely dependent on the desired outcomes of each individual study.
Qian said, “Our research lays the foundation for understanding the advantages and disadvantages of different approaches for generating patient-specific heart muscle cells for clinical implications, such as disease modeling, drug screening, and ultimately repairing human heart muscle after injuries, such as heart attacks.”
This work was funded by the National Institutes of Health, the American Heart Association, and the Ellison Medical Foundation.
Media Contact: Mark Derewicz, 984-974-1915, mark.derewicz@unchealth.unc.edu