A new bedside rounding approach will become standard for internal medicine teaching teams at UNC Medical Center. Last year, the Accreditation Council for Graduate Medical Education (ACGME) selected UNC as a funding recipient for Back to Bedside, a resident-led initiative to empower medical residents and fellows to increase time with patients, to improve both physician and patient well-being. Medicine residents won a grant to implement a multidisciplinary project. The pilot began in October 2017.
Led by second year resident Dr. Katie Haroldson, and chief residents Dr. Anthony Mazzella and Dr. Rosanne Tiller, The FaceTime Fraction: A Patient-Focused Shift in Emphasizing Empathic Communication and Multidisciplinary Rounding is currently being implemented in the department of medicine on five teaching teams and will be expanded to all internal medicine teams–with the exception of intensive care units.
The resident team has also designed a curriculum to teach physicians, nurses, care managers, pharmacists, and medical students how to implement the multidisciplinary approach. An educational booklet and series of teaching videos can be found here.
“We are refocusing the attention of the healthcare team to more actively engage the patient and care partners through improved communication and rounds efficiency,” said Haroldson. “The emphasis is on engaging everyone, the nurse, the pharmacist, the care manager and students, so that all can communicate clearly with the patient.”
The Pre-Round Huddle
A key curriculum video demonstrates a pre-round huddle, with the expectation that all members of the team have computer pre-rounded prior to team rounds. This includes the charge nurse and case manager, who can discuss pending discharges or concerns.
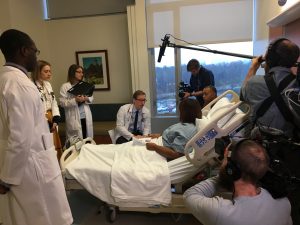
Dr. Mazzella says the main difference in rounding is that the discussion that traditionally occurred outside of a patient’s room, behind a closed door, is now inside the room, at eye level with the patient. Medical teams contact primary nurses to let them know they’ll be arriving to talk with a patient. Then, they enter the room. Demonstrated through video, the primary communicator, usually an intern physician, talks to the medical team and the patient about each active medical problem and the proposed plan for the day.
“A large part of this intervention is encouraging everyone, including supervising attending physicians, to complete a comprehensive review of patients on the electronic health record prior to discussion of the plan,” said Mazzella. “This way, each team member knows how care should progress on a given day. Then, rounds are a time to reconcile these thoughts as a team, with the patient.”
The team has also generated “Face Sheets” which include pictures and names of the providers for every patient.
The Inspiration for Back to Bedside
Haroldson says a universal discontent with the traditional rounding structure inspired the team to create the Back to Bedside project.
“Patients felt there was minimal face time with care teams and limited involvement in their care. Nurses felt excluded from rounds and were not considered part of the care team, while physicians felt disconnected with their patients, spending most of their time speaking outside of a closed door or sitting in front of a computer screen. This collective input inspired us to design the new rounding structure.”
Medicine residents are currently tracking post-implementation surveys for residents, nurses, and attendings. Patient satisfaction scores are being followed pre- and post-implementation through an HCAHPS survey. Early nurse and physician feedback has been positive.