Under the direction of assistant professor of radiology Li-Ming Hsu, the research demonstrates how long-term cocaine use affects brain functions, making recovery and stifling cravings more difficult.
A collaborative research endeavor by scientists in the Departments of Radiology, Neurology, and Psychology and Neuroscience at the UNC School of Medicine have demonstrated the deleterious effects of chronic cocaine use on the functional networks in the brain.
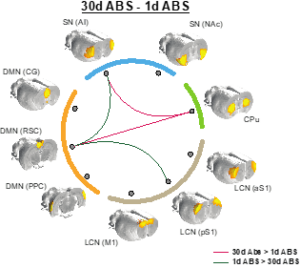
Their study titled “Network Connectivity Changes Following Long-Term Cocaine Use and Abstinence”, was highlighted by the editor of Journal of Neuroscience in “This Week in The Journal.” The findings show that continued cocaine use affects how crucial neural networks communicate with one another in the brain, including the default mode network (DMN), the salience network (SN), and the lateral cortical network (LCN).
“The disrupted communication between the DMN and SN can make it harder to focus, control impulses, or feel motivated without the drug,” said Li-Ming Hsu, PhD, assistant professor of radiology and lead author on the study. “Essentially, these changes can impact how well they respond to everyday situations, making recovery and resisting cravings more challenging.”
Hsu led this project during his postdoctoral tenure at the Center for Animal MRI in the Biomedical Research Imaging Center and the Department of Neurology. The work provides new insights into the brain processes that underlie cocaine addiction and creates opportunities for the development of therapeutic approaches and the identification of an imaging marker for cocaine use disorders.
The brain operates like an orchestra, where each instrumentalist has a special role crucial for creating a coherent piece of music. Specific parts of the brain need to work together to complete a task. The DMN is active during daydreams and reflections, the SN is crucial for attentiveness, and the CEN, much like a musical conductor, plays a role in our decision-making and problem-solving.
The research was motivated by observations from human functional brain imaging studies suggesting chronic cocaine use alters connectivity within and between the major brain networks. Researchers needed a longitudinal animal model to understand the relationship between brain connectivity and the development of cocaine dependence, as well as changes during abstinence.

Researchers employed a rat model to mimic human addiction patterns, allowing the models to self-dose by nose poke. Paired with advanced neuroimaging techniques, the behavioral approach enables a deeper understanding of the brain’s adaptation to prolonged drug use and highlights how addictive substances can alter the functioning of critical brain networks.
Hsu’s research team used functional MRI scans to explore the changes in brain network dynamics on models that self-administrated cocaine. Over a period of 10 days followed by abstinence, researchers observed significant alterations in network communication, particularly between the DMN and SN.
These changes were more pronounced with increased cocaine intake over the 10 days of self-administration, suggesting a potential target for reducing cocaine cravings and aiding those in recovery. The changes in these networks’ communication could also serve as useful imaging biomarkers for cocaine addiction.
The study also offered novel insights into the anterior insular cortex (AI) and retrosplenial cortex (RSC). The former is responsible for emotional and social processing; whereas, the latter controls episodic memory, navigation, and imagining future events. Researchers noted that there was a difference in coactivity between these two regions before and after cocaine intake. This circuit could be a potential target for modulating associated behavioral changes in cocaine use disorders.
“Prior studies have demonstrated functional connectivity changes with cocaine exposure; however, the detailed longitudinal analysis of specific brain network changes, especially between the anterior insular cortex (AI) and retrosplenial cortex (RSC), before and after cocaine self-administration, and following extended abstinence, provides new insights,” said Hsu.
Media contact: Kendall Daniels, Communications Specialist, UNC Health | UNC School of Medicine